New user registration rules do not result in loss of access to the NHS, states ACSS
The ACSS clarifies that new NHS registration rules, aimed at updating inactive user lists, will not result in a loss of healthcare access for patients.

Latest news and stories about patient care in daily life in Portugal for expats and residents.
The ACSS clarifies that new NHS registration rules, aimed at updating inactive user lists, will not result in a loss of healthcare access for patients.

The article advocates for equitable access to biologic treatments for patients with severe asthma, emphasizing the need to update Ordinance No. 261/2024/1 to ensure that these patients receive the same level of care as those with other chronic conditions. It frames this issue as an ethical and social imperative, highlighting the injustice faced by asthma patients in accessing necessary medical treatments.

The number of patients without an assigned family doctor has increased, reaching 1.6 million in January. This rise is attributed to a growing demand for healthcare services, with an additional 231,000 patients in the NHS over the past year.
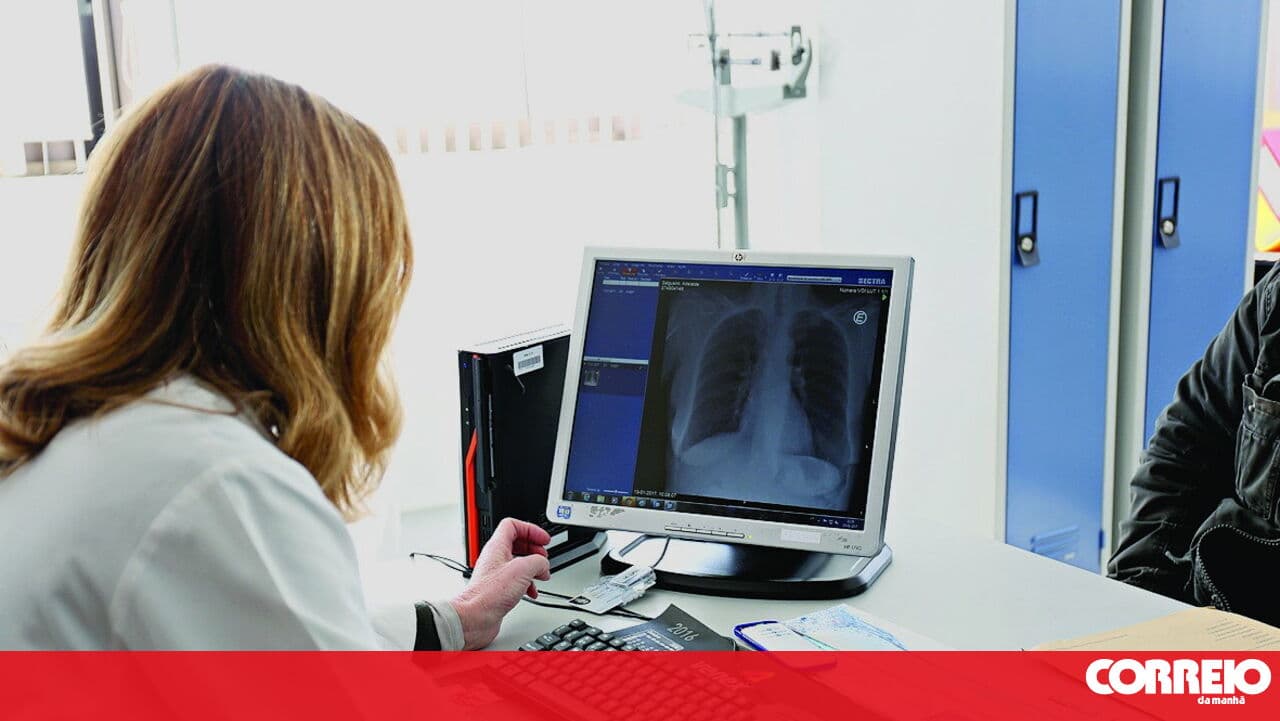
Mayors in Barreiro are opposing the closure of the obstetrics and gynaecology emergency unit, citing that over 16,000 births have occurred there between 2014 and 2024. They find the decision to close the unit incomprehensible, especially in light of ongoing healthcare challenges, such as ambulances being held for hours at other emergency departments due to high patient volumes.

Directors from leading cardiology services are advocating for the strengthening of existing cardiology centres rather than the establishment of new facilities. They argue that the creation of new reference centres undermines the current model established in 2023, as it does not significantly increase the system's capacity and may even weaken it.
Update: Opposition to New Facilities
Directors of three of the country's leading cardiology services have voiced their opposition to the opening of new reference centres, stating that the expansion of services “hardly increases the actual capacity of the system” and may even weaken it.

In 2025, over two thousand professionals retired from the NHS, raising concerns about the potential impact on patient care and public safety. Reports indicate that this mass retirement could lead to significant challenges in healthcare delivery, prompting calls for urgent reforms to address staffing shortages and ensure continued quality of care.

This article explains what clinicians and expectant mothers mean when they say paracetamol is “safe in pregnancy”. It clarifies that safety is relative: paracetamol is generally recommended as the first-line option for fever and mild-to-moderate pain because evidence from trials and guideline reviews shows a favorable risk–benefit profile compared with alternatives, but observational studies have suggested possible small associations with neurodevelopmental outcomes (eg, ADHD, ASD) that remain uncertain and may reflect confounding. Practical guidance is summarised: use the lowest effective dose for the shortest necessary time, avoid routine long-term or high-dose use, seek personalised advice from a healthcare professional (especially for repeated or high-dose use), and consider non-drug measures where appropriate. The piece emphasises evidence limitations, the importance of shared decision-making, and following national maternity-care guidance for expat and local patients alike.

Portuguese reporting indicates a sharp rise in monthly fees at some care homes — increases of roughly €500 — driven largely by a persistent labour shortage and higher operating costs. The hikes are prompting families to withdraw elderly relatives, intensifying pressure on informal care networks and raising equity and access concerns for vulnerable patients. Economically, the trend highlights how rising labour costs and constrained staffing can be passed directly to users in minimally regulated markets, with implications for social policy, funding models and workforce recruitment/retention. Separately, French coverage notes a demobilisation of farmers’ protests in Paris, underscoring a wider context of labour and sectoral tensions across services and primary production.

Despite repeated technical assessments, confirmed financial capacity and clear structural proposals, the SNS and INEM keep failing to deliver timely emergency responses. This analysis points to implementation gaps — weak governance, fragmented coordination between national and regional bodies, staffing shortages and poor resource allocation — rather than lack of solutions; the result is delayed care that harms patients (including expats) and undermines public wellbeing. Addressing the problem requires transparent accountability, an independent audit of operational bottlenecks, data-driven redistribution of resources and political commitment to implement already-defined reforms.

A Nova SBE report, 'Self‑medication in Portugal: Practices, Determinants and Behavioural Profiles', finds that 51.85% of respondents have self‑medicated at some point. The practice is especially common among younger people, those with higher education and people without a family doctor, and is being used for mental health issues as well as physical complaints. Most people do not inform their doctor about self‑medication, prompting experts to warn of risks for mental health and for patients with chronic conditions. The study highlights gaps in access to primary care and the need for better patient education and reporting practices.

Difficulties accessing the National Health Service (SNS) are driving patients away from exclusive reliance on public care and toward private healthcare. More than half of people report self-medicating and the majority do not inform their doctor, while those who can afford private care rarely revert to the SNS once they switch. The trend suggests growing segmentation in access and a potential long-term shift of wealthier patients out of the public system.

A new report finds episodes of illness rising particularly among younger people in Portugal, contributing to an overall increase in the number of people falling ill while persistent barriers to accessing the SNS (Serviço Nacional de Saúde) remain high. The data suggest growing pressure on primary and urgent care, uneven access driven by geographic, capacity and administrative constraints, and possible underlying drivers such as changing infection patterns, mental‑health needs and disruptions to routine care. The report calls for targeted policy responses to expand capacity, improve outreach to younger cohorts and reduce practical barriers to care, and for more granular analysis to identify regional and demographic causes.

Emergency departments and hospitals are experiencing significant difficulty admitting patients presenting with respiratory problems, creating bottlenecks in patient flow and raising concerns about care delays and safety. The situation appears driven by high demand for acute respiratory care combined with constrained inpatient capacity, staffing pressures and infection-control requirements that limit bed availability. This strain on emergency and hospital services risks longer waits, compromised care coordination and wider impacts on public health and system resilience unless capacity or operational responses are implemented.

Rising influenza activity is increasing admissions to intensive care and placing growing pressure on emergency departments. Health authorities warn the epidemic has not yet peaked, and the country is experiencing higher-than-expected mortality for the season, raising concerns about healthcare capacity and the potential need for surge planning and resource prioritisation.

The Portuguese Firefighters' League (LBP) has established a weekend task force of four additional ambulances to bolster pre-hospital emergency response and ease pressure on hospitals. The emergency vehicles — drawn from the Ajuda, Cabo Ruivo, Camarate and Cascais brigades — will be based at the LBP headquarters, while a commander will be on permanent duty at CAASO (Centre for Operational Monitoring and Support) to coordinate operations. The deployment is a targeted, short-term capacity boost intended to improve response times during busy periods and provide centralised operational oversight.

Beja Hospital’s obstetrics and gynaecology emergency service will be closed overnight due to a shortage of doctors, operating from 20:00 on Saturday until 08:00 on Sunday and again from 20:00 on Sunday until 08:00 on Monday. The closures are attributed to an inability to complete the rota, raising concerns about patient access to urgent maternity and gynaecological care and potential pressure on neighbouring services. An accompanying opinion notes systemic failings in emergency logistics — exemplified by ambulances held up by missing stretchers — as symptomatic of wider incompetence in healthcare operations.
Carlos Enes of CNN Portugal examines recurring, serious failings in Portugal’s emergency response system, arguing that political and union attacks on INEM distract from patient safety. He urges giving INEM operational authority, requiring ULS hospitals to free trolleys and beds, and restoring clinical judgement as the primary guide for urgent care, while calling for systemic changes to protect public health.

Almost a year after the minister warned of unacceptable A&E waiting times, there has been no meaningful improvement. Persistent delays point to systemic strain on emergency services, heighten risks to patient safety and wellbeing, and indicate a need for urgent policy and resource interventions rather than repeated warnings.

Ten years ago, Garcia de Orta Hospital in Almada opened the first hospital-at-home unit. Today there are already 50 Local Health Units offering this service — a way of delivering healthcare to 400 patients receiving inpatient care outside the hospital.

CTT said the suspension of the reimbursement service for the Mobility Allowance for residents in the Azores and Madeira is due to 'reasons beyond the company's control'.
On Saturday the obstetrics and gynaecology emergency departments at the hospitals in Abrantes, Setúbal and Portimão, and the obstetrics emergency department in Vila Franca de Xira, will be closed. The Setúbal emergency department reopens on Sunday.
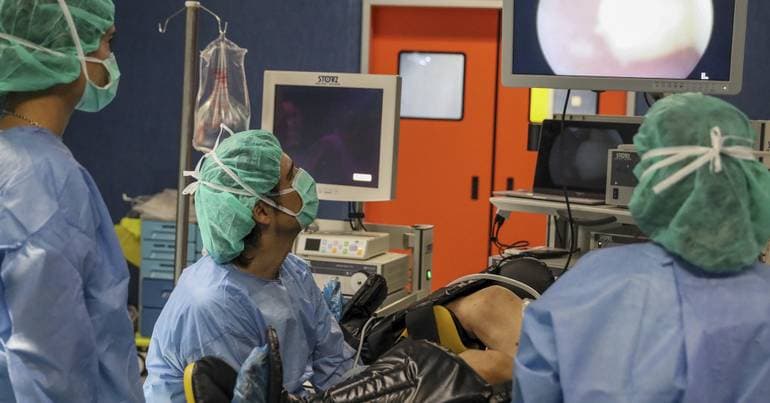
Today the terms of ten boards of directors of Local Health Units (ULS) across Portugal come to an end, including the board at Hospital de São José. Rosa Valente Matos, who has led São José for six years, said she was not given any justification for the decision not to renew her mandate. The SNS administration confirmed several appointments will not be renewed and noted that the São José post was awarded to a PSD-affiliated figure; its 18:00 bulletin also included an analysis of possible developments in conflicts in Eastern Europe and the Middle East, framing the personnel changes within wider political and policy considerations.

In 2025 SNS24 handled over 5.7 million calls and scheduled more than one million primary healthcare appointments — about 2,800 per day — frequently referring patients to same‑day or next‑day in‑person primary care. The data highlights SNS24’s expanding role in triage and in facilitating timely access to primary care through a telehealth appointment‑scheduling function.
Four gynaecology and obstetrics emergency departments have been closed. In Amadora‑Sintra only the gynaecology emergency department is shut; meanwhile the general emergency at Hospital Fernando Fonseca (Amadora‑Sintra) reported a three‑hour wait for patients classed as very urgent as of 20:00, according to the SNS Portal. Santa Maria recorded a two‑and‑a‑half‑hour wait for very urgent cases, and Hospital de Loures topped the waiting‑time list with around three‑hour waits for urgent patients.