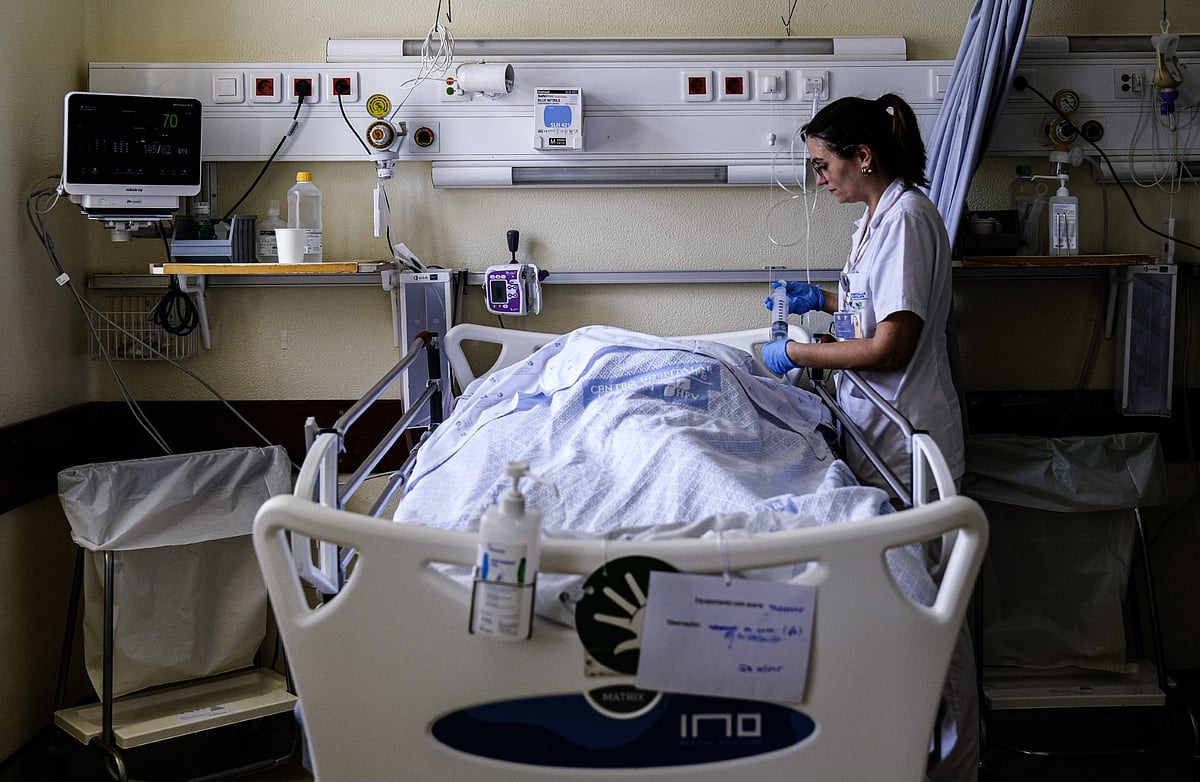
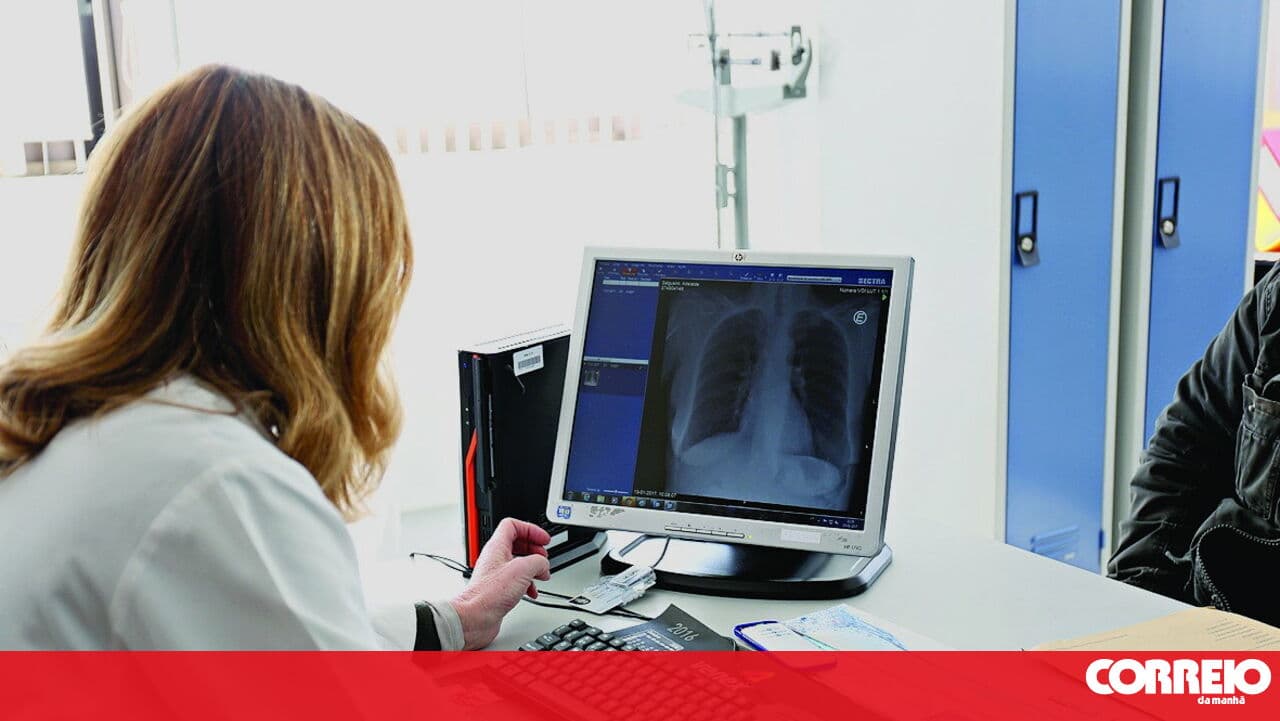
Majority of Portuguese concerned about public health system
A study by the Catholic University of Portugal indicates that nearly 70% of respondents are worried about the state of the National Health Service (Serviço Nacional de Saúde or SNS). Over a third of those surveyed reported needing private health insurance due to concerns regarding waiting lists and emergency response times. Critics argue that despite government pledges to maintain a universal public system, current policies are shifting focus toward private interests.
Staffing and shift schedules in the SNS combine permanent doctors, residents and temporary cover (locums or overtime) arranged by each hospital's Clinical Directorate ("Direção Clínica"), which plans rotas to cover on‑call and emergency shifts. Rotas are subject to national labour rules, collective agreements and local shortages, so hospitals may use voluntary shift swaps, incentives or external contractors when regular staff are unavailable.